
Have you ever had a gut feeling about something? Have you ever gotten butterflies in your stomach before a stressful event?
Those feeling aren’t just in your head (at least not entirely). Your brain is in constant communication with gut through something called the “gut-brain axis,” and this connection is a two way street. The brain (emotions, behavior, mood) influences the gut just like the gut (the food we eat, the microbiome, toxins) influences the brain.
Over the last several years, mounting evidence is pointing to a gut-brain link in children with neurological conditions like Autism, ADHD, Sensory Processing Disorder (SPD), and many other behavioral disorders.
Curious to know more? Keep reading for the full scoop on the crucial role that gut health plays in the development and treatment of special needs.
What is the Gut Microbiome?
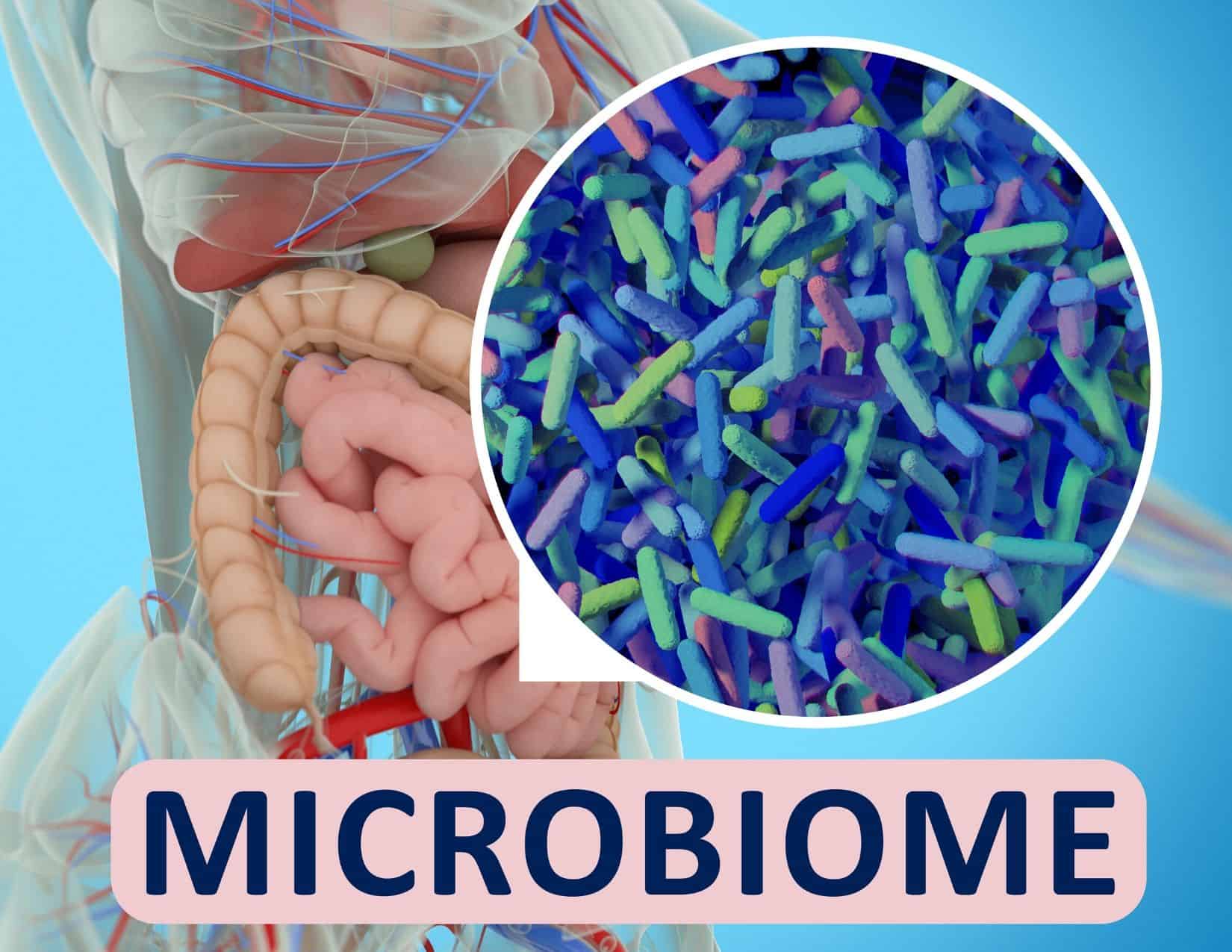
Thousands of years ago, Hippocrates said that “all disease begins in the gut.” It’s taken medical research quite some time to catch up, but thanks to the launch of the Human Microbiome Project by the NIH, we now have evidence that most (if not all) chronic diseases do originate in the gut. [1]
What’s so special about the gut?
The human body is home to trillions of microbial organisms, including bacteria, viruses, and fungi—but the largest concentration is in the gut. We have over 1,000 different microbial species living in the gut.
From a genetic and cellular perspective, we’re more bacterial than we are human. Bacterial cells outnumber human cells 10:1 and bacterial genes outnumber human genes 150:1! Based on this data, it’s not surprising that our microbial genes have a bigger influence on our health than our own genes.
What are these microbes up to all day (and night)?
- Regulating the immune system
- Eliminating toxins
- Regulating metabolism
- Controlling appetite
- Producing nutrients (Vitamin K2, B12, etc.)
- Digesting foods
- Producing short-chain fatty acids
- Regulating hormones
- Producing neurotransmitters (serotonin, dopamine, GABA)
- Controlling inflammation
- Regulating sleep
- Influencing mood and behavior
It’s probably a good time to point out that we have both good and bad bacteria living in our gut. And some of the species fall into a grey area where they can be beneficial in certain amounts and harmful in other amounts. More on that later. Let’s move on to where these microbes come from…
Where Do We Get Our Microbiome From?

Scientists used to believe the womb was sterile with no bacterial cells whatsoever. Now, we know that the “seeding” of the microbiome starts when babies are still in utero. [2] But, by far, the biggest establishment of the microbiome is at birth.
Unfortunately, the evidence isn’t good for babies born via Caesarian section. When babies go through the vaginal canal, they’re inoculated with microbes from their mother. When babies miss this critical step, they end up with a microbiome that resembles the hospital environment and is dominated by opportunistic pathogens like Enterococcus and Klebsiella rather than the commensal strains found in healthy guts. [3]
Epidemiological studies show that babies born via C-section have increased risks of type 1 diabetes, asthma, obesity, and other health problems later on in life. [4]
To counteract this, many families are choosing to swab babies born by c-section with vaginal fluids to help seed the microbiome. [5]
Breastfeeding and skin-to-skin care with babies can also help to establish a healthy microbiome since breastmilk is full of both prebiotics and probiotics. The skin also has a microbiome, so doing skin-to-skin with family members can help to transfer microbes from both Moms and Dads too.
By a year of age, babies’ microbiomes start to closely resemble their parents’ microbiomes (which is why it’s important for parents to prioritize gut health before pregnancy). By the age of 3, children have their full adult microbiome. [6] Interestingly, this is also the age that many neuro-developmental disorders like Autism, ADHD, and SPD emerge.
Now that we know a little more about the microbiome, let’s move on to how the gut and brain communicate.
What is the Gut-Brain Axis?
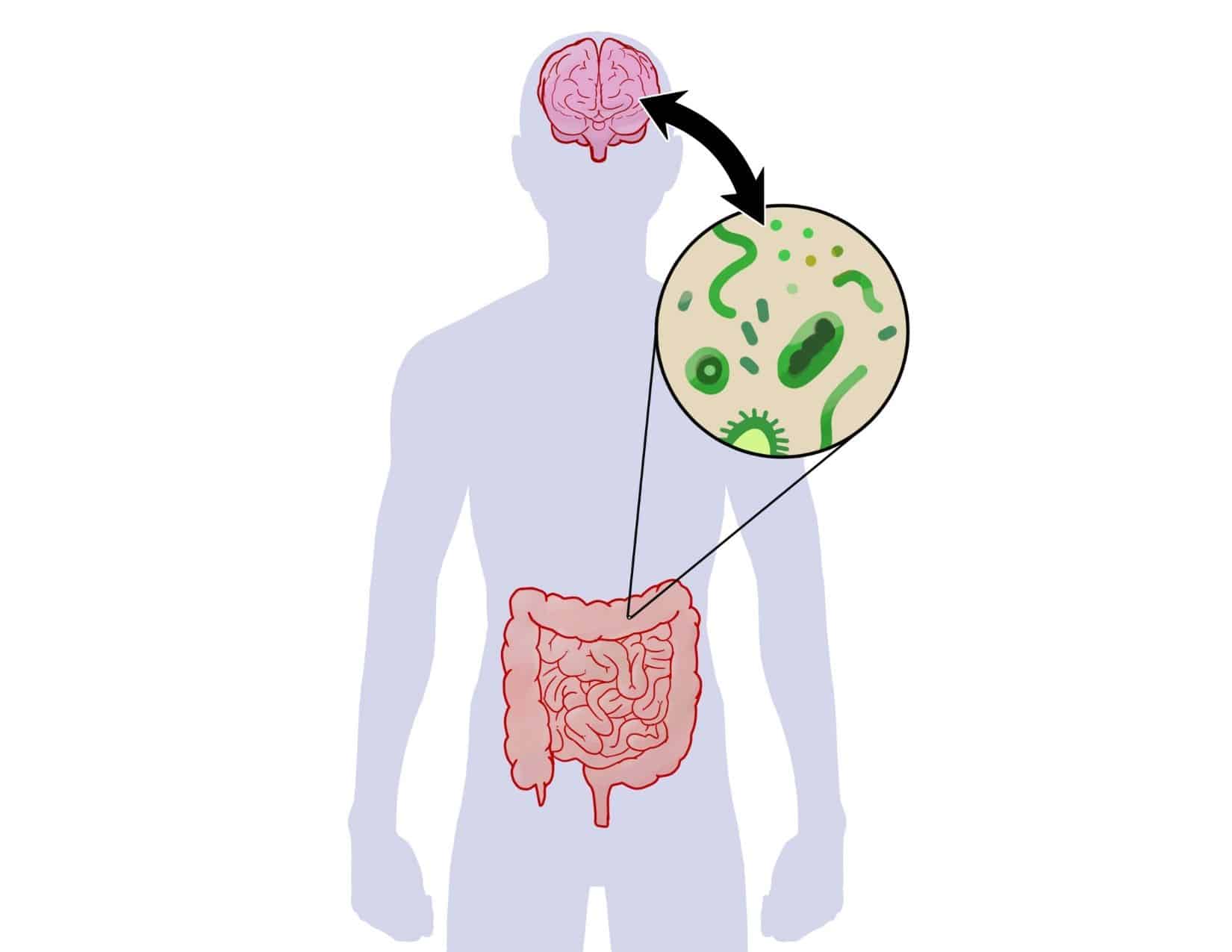
The gut-brain axis is often called the “second brain.” In reality, I think the microbiome is the first brain, the gut itself is the second brain, and the brain in our heads is our third brain. (That’s a lot of brains!)
When people talk about the gut-brain axis, what they’re really referring to is the enteric nervous system (ENS). This encompasses the neurons that cover the whole digestive tract (from where food enters to where it exits) and it regulates the entire GI tract via the vagus nerve that goes directly to the brain.
This is an incredibly complex and unique nervous system since it’s the only one in the body that can operate independently (without input from the central nervous system). The ENS also has more nerve endings than anywhere else in the body and more nerve tissue than the spinal cord. No wonder you get gut feelings about things!
The gut-brain axis is really like an information superhighway that is exchanging information back and forth all the time. They talk about things like hunger, fatigue, stress, and even give information about the microbiomes around us. That’s right—your microbiome can “read” other peoples’ microbiomes and influence how you feel about them. [7] They may even play a role in choosing mates! [8]
Bacteria in the gut can send direct messages to your brain that influence how you feel. A happy gut = a happy brain. Many “happy” chemicals are produced in the gut, including serotonin, dopamine, and GABA.
When you have gut dysbiosis (too many bad bacteria and not enough good), the traffic lights that regulate the communication superhighway between your gut and brain stop working, and your entire body goes into chaos. Your physical, mental, and emotional health begins to suffer.
Some of the signs of gut dysbiosis are:
- Upset stomach
- Bloating
- Nausea
- Constipation
- Diarrhea
- Rectal or vaginal itching
- Problems with urination
- Bad breath
- Headaches
- Joint pain
- Allergies
- Acne
- Chest pain
- Rashes
- Fatigue/lethargy
- Difficulty concentrating
- Depression
- Anxiety
- Mood swings
- Trouble sleeping
- Behavioral issues in children
- Sensory issues
What is the Link Between Special Needs and Gut Health?
The Link Between Autism and the Gut Microbiome

A lot of the initial research about Autism (ASD) focused on genetics and brain health. Now, we know that there are many factors that contribute to the disorder. Current research points to environmental toxins, diet and metabolic status, genetics, the immune system, inflammation, and the microbiome.
Up to 70% of kids with ASD also suffer from GI symptoms like constipation, diarrhea, stomach pain, and more. [9] Many studies have found that children on the spectrum have gut dysbiosis. [10]
One meta-analysis that included 247 children with Autism found that these kids had lower amounts of certain strains of bacteria like Akkermansia, Bacteroides, Bifidobacterium, and Parabacteroides and a higher amount of Faecalibacterium compared to neurotypical children. Kids on the spectrum also had less Enterococcus and Escherichia coli and higher amounts of Lactobacillus. [9]
Other studies have also found that many children with Autism have higher levels of certain Clostridium strains. [11] In one study, levels of Clostridium paraputri, Clostridium bolteae, and Clostridium perfringens were higher than in neurotypical children. The children with ASD also had two strains of Clostridium that weren’t found in neurotypical children at all. [12]
Pesticide exposure during pregnancy is a known risk factor for Autism. [13] It’s no secret that one of the most wide-spread herbicides is glyphosate, the main ingredient in Roundup. In the United States alone, over 300 million pounds of this herbicide is sprayed yearly making it nearly impossible to avoid exposure.
Recent research has shown that glyphosate destroys good bacteria in the gut while allowing harmful strains (like Clostridium) to grow. [14] In addition to increases in cancer, many experts believe there is a direct correlation between the use of glyphosate and the increase in Autism. [15]
In some cases, a two-week, high dose of antibiotic therapy to wipe out 95% of the microbiome and a subsequent fecal microbiota transplant (FMT) alleviates gastrointestinal and ASD symptoms. [16] If you’re not familiar with FMT, it involves transplanting a healthy microbiome from a sample of poop into an unhealthy microbiome to re-culture it with beneficial bacteria. (Please note that this should only be performed by trained medical experts and never attempted at home.)
We definitely need more long-term research on fecal microbiota transplants for kids with Autism, but experts believe it could be a promising treatment. [17]
If you’re interested in more info on fecal microbiota transplantation, check out OpenBiome.
The Link Between ADHD and the Gut Microbiome

ADHD is a neurodevelopmental disorder that’s associated with abnormalities in dopamine signaling (a neurotransmitter in the brain) and differences in reward processing. Similar to ASD, children and adults with ADHD have some changes in their microbiome that could point to a gut-brain link.
One study found that people of all ages with ADHD had higher levels of Bifidobacterium than controls and that this may correlate with changes in dopamine signaling and reward processing. [18]
Another study found that teenage males with ADHD had less overall microbial diversity and increased levels of Bacteroidaceae, and both Neisseriaceae and Neisseria species than controls. [19]
The gut-brain link is still a new theory for the origin of ADHD, but many researchers believe it is one that’s worth exploring. More and more scientists are pointing to the development of ADHD in the gut, not the brain. [20]
The Link Between Sensory Processing Disorder and the Gut Microbiome

Sensory Processing Disorder (SPD) is more prevalent than Autism and about as common as ADHD. It is very similar to these disorders and many kids share a combination or all three of these disorders (which is why it isn’t surprising that there’s a lot of overlap).
Scientists believe the gut microbiome may play a role in the brain’s development, likely through the gut-brain axis. Recently, a study on children with SPD found that the back of the brain contained abnormal white matter tracts in areas that function as important connections for auditory, visual, and somatosensory (touch) processing, including the connections between the left and right sides of the brain. [21] This is different from children with Autism and ADHD who tend to have more tracts in the frontal areas of the brain.
Interestingly, your gut processes sensory input first, then sends a message about it to your brain. Children with Sensory Processing Disorder often have high levels of anxiety and view sensory input as stressful. Emerging research shows that there is a link between stress response and the gut microbiome. [22]
One of the ways that the gut helps to manage stress and anxiety is through the production of neurotransmitters. One example of a calming neurotransmitter that’s produced in the gut is GABA. Altered production of GABA has been associated with anxiety, depression, and even perception of pain. [23]
Glutamate is another neurotransmitter produced by the gut and is a precursor for GABA. Glutamate is particularly interesting for kids with SPD because it helps to regulate the sensory system and how the brain processes sensory input. Too much or too little glutamate could have a huge impact on sensory regulation.
While we still need research to investigate a link between the microbiome and Sensory Processing Disorder, there’s a lot of evidence that the gut-brain axis plays a role.
How Does Leaky Gut Impact Autism, ADHD, and SPD?
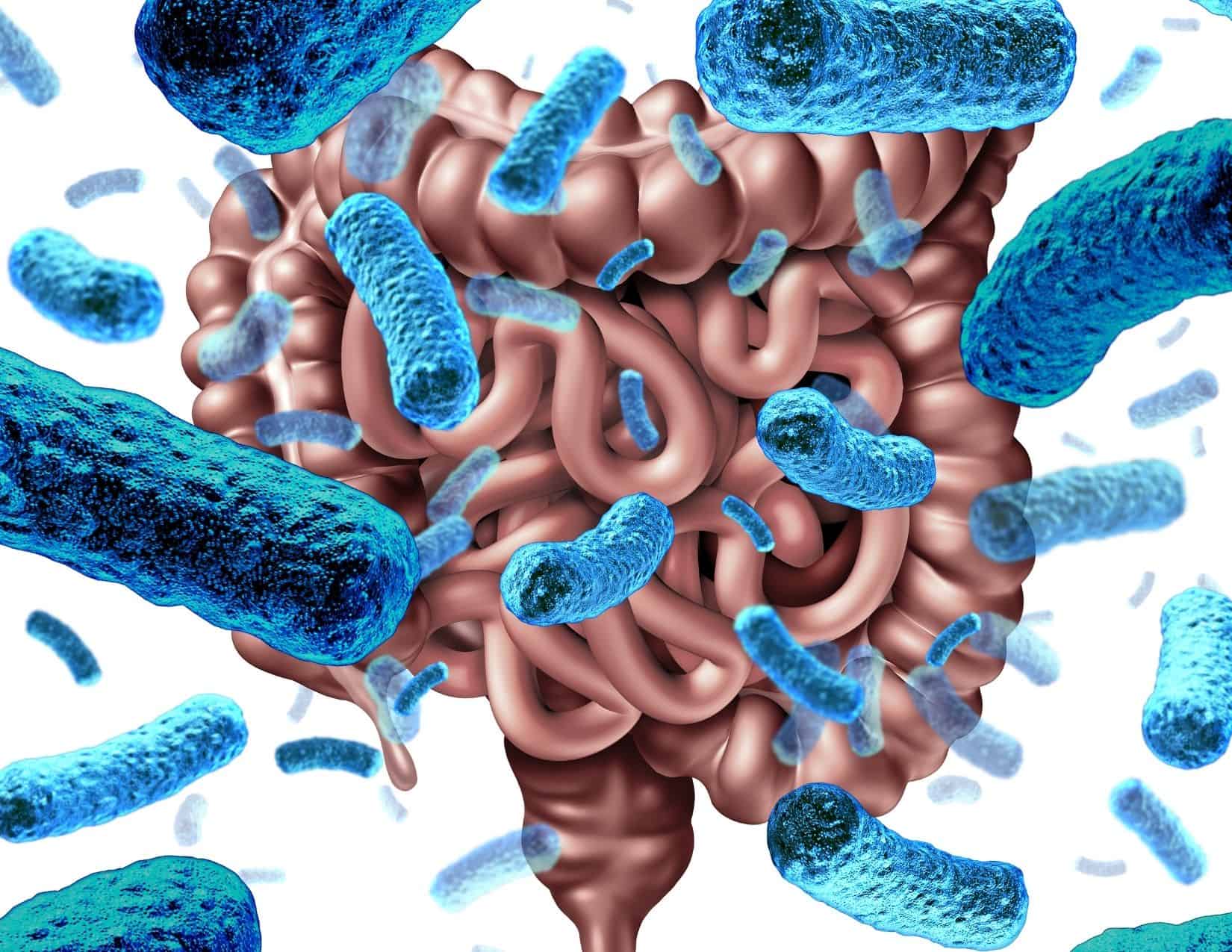
The medical term for leaky gut is “intestinal permeability.” In a healthy gut, there are tight junctions that regulate what passes through the lining of the small intestine. If these junctions are damaged and become leaky, larger particles of undigested food, proteins, toxins, and even harmful bacteria may enter the bloodstream.
Intestinal permeability has been associated with many diseases, including ulcers, diarrhea, IBS, Celiac, inflammatory bowel disease, allergies, obesity, diabetes, cancer, and more. [24] Research is also pointing to a link between leaky gut and Autism, ADHD, and SPD.
We talked earlier about how Clostridium levels are increased in children with ASD. Studies have found that Clostridium can harm the intestinal lining and lead to leaky gut. [25]
Studies have shown that children with ASD have increased levels of zonulin, a marker of intestinal permeability. [26] Another study showed that 43% of children with Autism had leaky gut while none of the controls did. [27] Other studies have found similar findings in children with ADHD and other mental health conditions. [28]
How does leaky gut contribute to Autism, ADHD, and SPD?
First, we need to start with something called the “blood-brain barrier.” Similar to the tight junctions in the lining of the small intestines, the brain has a selective barrier that regulates what passes from the blood into the brain. This barrier is designed to allow vital nutrients to reach the brain while keeping out toxins and other harmful substances.
Scientists now know that commensal bacteria (healthy bacteria found in the general population) are necessary for the development of the blood-brain barrier. [29] They have also discovered that changes in the microbiome and increased intestinal permeability can lead to increased permeability of the blood-brain barrier. [30]
In a sense, leaky gut = leaky brain.

Research has shown that ASD is also associated with an altered blood-brain barrier and inflammation of the brain. [31] This may explain why children with neurodevelopmental conditions are more susceptible to toxins in food, the environment, medications, vaccines, etc.
The toxins literally have direct access to the brain!
Leaky gut can also increase food allergies and intolerances because large, undigested molecules of food enter the bloodstream where the immune system marks them as foreign. This means that every time the immune system sees those same molecules again, they mount an immune attack (an allergic reaction).
“Metabolic endotoxemia” is the term used to describe what happens in the body when someone with leaky gut eats a meal (especially meals high in calories and fat). [32] Toxins and particles that aren’t supposed to be in the blood enter the bloodstream through the lining of the intestines and create “toxemia” in the blood. This causes long-term inflammation and has been associated with many chronic diseases.
Not surprisingly, metabolic endotoxemia can also cause inflammation in the blood-brain barrier.
How Does Candida Impact Gut and Brain Health?

Just like we have both good and bad bacteria in the gut, we also have good and bad types of yeast in the gut. Candida is a normal yeast living in the gut, but when certain strains grow in abundance, it can cause yeast overgrowth. Candida albicans is one of the most well-known types of yeast that causes the infection, Candidiasis.
In one study, an overgrowth of Candida was found in 57.5% of children with ASD but not in any of the controls. [33] Another study identified three different strains of Candida in the stools of children with Autism, the most abundant being Candida albicans. [34] In a case study of an individual suffering from ADHD and depression, treating a Candida infection with olive leaf extract improved symptoms. [35]
Yeasts like Candida feed on sugar and carbohydrates. Many children with Autism, ADHD, and SPD have very limited diets that are high in sugar and carbs. It becomes a chicken and egg scenario, because yeast infections lead to sugar cravings and excess sugar can lead to yeast infections.
Some of the signs of Candida overgrowth include:
- Hyperactivity
- Inappropriate laughter
- Inattention
- “Foggy” brain
- Self-stimulatory behavior
- Sensory impairment
- Fatigue
- Headaches
- Confusion
- Sleep disturbances
- Anger
- Aggression
- Crying episodes
- Constipation
- Stomach pain
- Bloating/gas
- Bed wetting
- Thrush in the mouth (white film)
- Diaper rash
- Eczema
- Red ring around the anus
- Cracking or rashes between the toes
- Rectal or vaginal itching
Does Diet Matter for Autism, ADHD, and SPD?

Yes! In the words of Hippocrates, “let food be thy medicine.”
A healthy diet has the ability to increase beneficial bacteria in the microbiome, repair leaky gut, reduce Candida overgrowth, and influence mood and behavior. On the other hand, an unhealthy diet can increase harmful bacteria in the gut, cause leaky gut, cause Candida overgrowth, and negatively influence mood and behavior.
Studies have found that many children with Autism, ADHD, and SPD suffer from micronutrient deficiencies. Supplementing with the right vitamins and minerals can help (check out my fav here), but correcting the diet will go further than any supplement ever can.
There’s a lot of evidence that food dyes and other artificial ingredients can lead to behavioral issues in children. We also know that many children on the spectrum suffer from multiple food allergies and intolerances.
Many parents of kids with conditions like Autism, ADHD, and SPD try diets like the Specific Carbohydrate Diet (SCD), GAPS, Paleo, Keto, or Gluten-free/Casein-free. What all of these diets have in common is the elimination of all foods containing gluten and casein.
Why should kids on the spectrum avoid gluten and casein?
- Gluten contains zonulin, which causes intestinal permeability (leaky gut)
- Wheat (gluten) and dairy (casein) are two of the top allergens, and allergies contribute to leaky gut
- Gluten and casein can cause folate deficiency and folate is necessary for brain development
- Gluten and casein cause an opioid-like reaction in the brain
- Gluten and casein decrease GABA and increase glutamate
- Gluten and casein increase inflammation in the body and the brain
Studies on gluten and casein-free diets for kids with ASD show that they work! [36, 37, 38, 39]
Changing the diet can be tough, especially if your child is a picky eater! In the resources section at the bottom, I’ll share my favorite tool for changing the diet and helping picky eaters expand their food selection.
What Role Do Probiotics Play?

Probiotics are beneficial strains of bacteria that have a positive effect in the gut (and subsequently the entire body).
Some of the benefits of probiotics include improving GI barrier function (preventing leaky gut), producing antimicrobial agents (natural antibiotics against pathogenic organisms), strengthening immunity, and altering the composition of bacteria in the microbiome. [40]
Multiple studies have confirmed that both prebiotic (food for bacteria) and probiotic therapy can improve GI and Autistic symptoms in children with ASD. [41, 42]
A very interesting study took 75 infants and randomized them into two groups: one received probiotics and the other didn’t. The researchers followed the infants for 13 years and found that 17.1% of the children who did not receive probiotics were diagnosed with either Autism or ADHD. In the group that did receive probiotics as infants, none of the children received either diagnosis. [43]
There aren’t many research studies on Sensory Processing Disorder in general, so there isn’t any data on the use of probiotics for kids with SPD. But, we do know that SPD is associated with anxiety, and studies have found a link between probiotics and the treatment (and prevention) of depression and anxiety. [44]
The Best Probiotics for Autism, ADHD, and Sensory Processing Disorder
By now, I hope that you can see the importance of gut health in kids with neurodevelopmental conditions.
A recent article titled “A Revolutionizing Approach to Autism Spectrum Disorder Using the Microbiome” summed it up nicely when it concluded that:
“diet and probiotics are seemingly promising breakthrough interventions in the context of ASD for lesser known side effects, feasibility and easier administration.” [45]
Before you go running to your local health food store for some probiotic gummies, we need to address quality and availability when it comes to probiotics. Not just any probiotics will do.
To be effective, probiotics need to be able to survive processing, the harsh acidic environment of the stomach and bile acids and colonize in the gut. Unfortunately, not many do. A study of eight leading probiotics found that only one was able to survive these harsh conditions. [46]
Another study of sixteen commercially available probiotics found that only one contained what the label said. For the others, there were differences between pill-to-pill and bottle-to-bottle. [47]
I’ve tried a lot of different probiotics over the years, and now I only stick with one. The probiotics I use are found in nature, not manufactured in a lab. They are called “spore-based probiotics” which means they exist in spore form until they reach your gut.
Spore-based probiotics can survive the GI tract and come alive in your gut. They have the ability to change the microbiome, improve intestinal permeability, kill harmful pathogens, and even produce antioxidants that can go to work right away in the gut. The best part is that these probiotics have undergone multiple studies that can back up these claims! [48, 49, 50, 51, 52, 53, 54, 55, 56, 57]
These specific spore-based probiotics were commercially formulated by Microbiologist, Kiran Krishnan. They are available through his two companies, Just Thrive Probiotics or Microbiome Labs. Just Thrive’s Probiotic contains a slightly lower dose of spores than Microbiome Lab’s Megasporebiotic.
Anyone can order from Just Thrive, but Megasporebiotic is a clinical dose of spores and can only be ordered through natural practitioners like myself.
I’ve included links in the resources section for both (plus a special discount code)!
Resources and 8 Steps to Improve Gut Health
- Learn the top 12 ways to improve the microbiome
- Incorporate kid-friendly probiotic foods into the diet
- Have your child’s gut health tested
- Learn how to transition to a gluten-free/casein-free diet and improve picky eating
- Supplement with nutrients designed for kids on the spectrum
- Order Just Thrive Spore-Based Probiotics (use the discount code holfam10 to save an additional 10% off)
- OR…Order Microbiome Labs Megasporebiotic (use patient direct code “holfamily”)
- Check out our other articles on holfamily.com













